Dilute Russell Viper Venom Time [dRVVT]
Introduction & Principle
Russell's viper venom [RVV] isolated from the snake Daboia russelii [or russellii - the correct spelling is a matter of great debate!] contains a potent activator of Factor X which in the presence of Phospholipid [PL], Prothrombin and calcium ions clots fibrinogen to fibrin. In individuals with a Lupus Anticoagulant [LA], the antibody binds to the phospholipid inhibiting the action of the RVV and prolonging the clotting time.
As the RVV directly activates Factor X, the test is unaffected by deficiencies of Factors XII, XI, IX or VIII. The dRVVT is frequently combined with a platelet neutralisation procedure to demonstrate the phospholipid specificity of the antibody.
The international recommendations for screening for a Lupus Anticoagulant, recommend two tests that employ different principals. Currently the ISTH SSC working party on Antiphospholipid Antibodies recommends the Silica Clotting Time [SCT] and the dilute Russell Viper Venom Time [dRVVT].
Method
Pooled normal plasma is mixed with diluted PL at 37°C. Diluted RVV and then Calcium chloride are added and the clotting time is measured. The test is then repeated using patient plasma and the ratio of test:normal plasma is calculated.
| Reagent | Explanation |
|---|---|
| Platelet poor Plasma | A source of coagulation factors, particularly Thrombin and Fibrinogen. |
| Dilute Russell's Viper venom | Typically this is diluted to give a clotting time in normal plasma of between 30-35s as this optimises sensitivity to antiphospholipid antibodies.
|
| Phospholipid | To provide a surface for Thrombin generation. This should be diluted to a sufficient degree that it becomes the rate limiting step and any inhibition by a LA prolongs coagulation. |
| Calcium | To initiate coagulation |
Interpretation
If the DRVVT is not prolonged then the correction test (sometimes referred to as the neutralisation test) is not indicated. However not all LAs will detected by the dRVVT and therefore the recommendations are to employ a second test using different principles ie the Silica Clotting Time [SCT].
| DRVVT | Interpretation |
|---|---|
| DRVVT Ratio [Test DRVVT/control DRVVT] |
Reference Range: 29-42s Reference Ratio: 0.9-1.05 |
| Ratio [Test DRVVT/control DRVVT] >1.05 | Possible LA Exclude deficiencies of factors II, V, X, fibrinogen or another non-LA inhibitor |
| Prolonged DRVVT which corrects with normal plasma | Clotting factor deficiency A weak LA can sometimes be masked in a 1:1 mix with normal plasma and some labs recommend a 1:4 mix [Normal plasma:Test plasma] to try and minimise this. |
| Prolonged DRVVT which corrects with PL | Lupus Anticoagulant |
Calculating the percentage correction:
A number of approaches have been used to calculate the percentage correction:
1. Using the formula below where '+ PL' is the dRVVT with additional phospholipid i.e. the neutralisation step.

2. A normalised correction The percentage correction of the ratio is calculated using the formula below where again '+ PL' is the dRVVT with additional phospholipid. The final result is multiplied by 100 to covert it into a percentage.
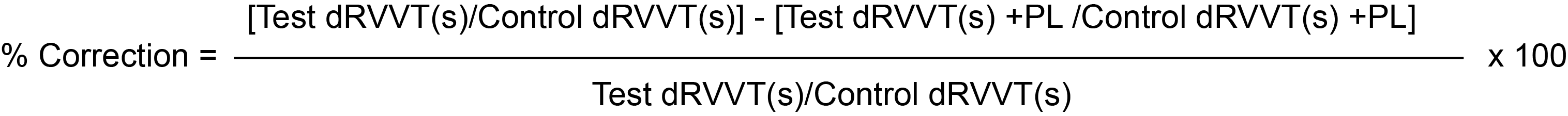
This latter calculation is that currently recommended by the British Committee for Standardisation in Haematology [BSH.]
In the following example:
| Sample | dRVVT Clotting Time [s] | Ratios |
|---|---|---|
| Patient Plasma | 69.2 s | [Patient Plasma]/[Control Plasma] = 1.82 |
| Control [Normal] Plasma | 37.9 s | |
| Patient Plasma + PL | 39.5 s | [Patient Plasma + PL]/ Control [Normal] Plasma + PL] = 1.21 |
| Control [Normal] Plasma + PL | 32.5 s |
From the data above: [1.82 - 1.21/1.82] x 100 = 33.5% correction. So in a patient in whom the dRVVT is prolonged as in this case [69.2s] the 33.5% correction is consistent with the presence of a Lupus Anticoagulant.
3. What constitutes a positive correction ratio? Most laboratories regard a correction of >10% with PL as being a positive test.
What Test Next
In individuals in whom a LA is identified, the test should be repeated in 12 weeks. It should also be remembered that not all tests including the dRVVT will identify all LAs and therefore, if the index of suspicion that a specific patient has a LA then other tests should be undertaken e.g. Silica Clotting Time [SCT]. Finally - the causes of a LA should be screened for e.g. ANA, drugs, viruses etc.
